Heart Surgery Approach Estimator
Select the options that best describe your potential procedure to see an estimated surgical approach.
--
--
You’ve probably heard the horror stories. A friend’s relative went in for a valve replacement and came out with a chest that looked like it had been through a demolition derby. You ask if they broke their ribs, and the answer is usually a grim nod. It’s no wonder you’re worried. The image of surgeons sawing through your chest bone is terrifying.
Here is the short answer: No, they do not break your ribs. Not intentionally, and certainly not by smashing them with a hammer. However, yes, they still split the breastbone (sternum) for most traditional open-heart surgeries. This procedure is called a median sternotomy. It has been the gold standard for decades because it gives surgeons the best possible view and access to the heart.
But medicine moves fast. Just because it was done this way in 1980 doesn’t mean it’s the only way today. In fact, depending on what exactly needs fixing inside your chest, you might not need your sternum split at all. Let’s look at what actually happens during surgery, why the "rib-breaking" myth persists, and when you can avoid the big incision entirely.
The Myth of "Broken Ribs": What Actually Happens?
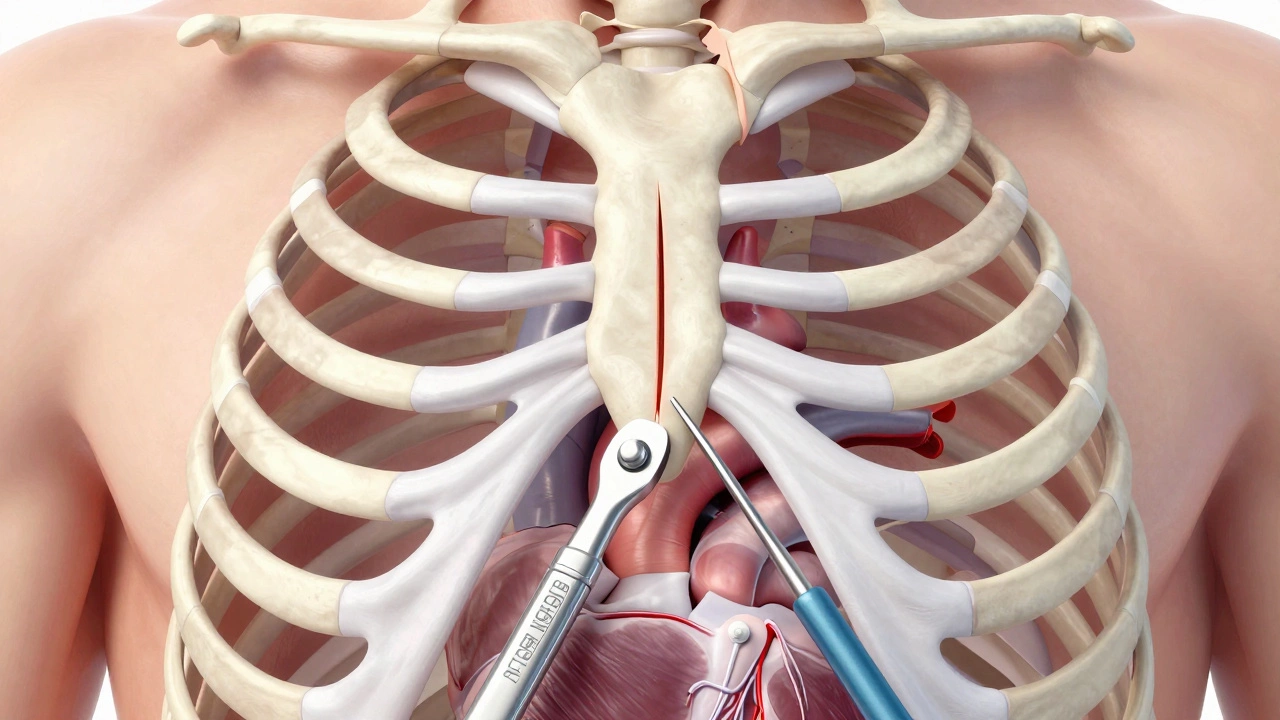
First, let’s clear up the anatomy. When people say "breaking ribs," they are usually confusing two different bones. Your ribs curve around your lungs like a cage. Your sternum is the flat bone right in the center of your chest that connects those ribs together.
In a traditional median sternotomy, which is the surgical splitting of the sternum to access the heart, surgeons use a specialized oscillating saw to cut straight down the middle of the sternum. They lift the two halves apart using a retractor. This provides a wide, open window to see the heart, the aorta, and the major vessels.
After the surgery is done, the surgeon puts the sternum back together. They don’t use glue or stitches alone. Instead, they wrap thin wires-usually stainless steel or titanium-around the bone and twist them tight to hold it in place while it heals. This process is called sternal wiring.
So, technically, the bone is cut, not broken by trauma. But from the patient’s perspective, it feels similar. The healing time for a sternotomy is significant. You have to protect your chest for about six to eight weeks. No lifting heavy objects, no pulling yourself up from a chair, and definitely no driving until your doctor clears you. The pain is real, but it is manageable with modern pain protocols.
Why does the "broken rib" myth stick? Sometimes, during complex surgeries or resuscitation efforts (like CPR), ribs can fracture due to pressure. Also, if a patient has severe osteoporosis (weak bones), the sternum might crack slightly during the initial cutting or closing. But in a standard, healthy adult undergoing elective heart surgery, the ribs themselves remain intact. The injury is to the sternum, and it is a controlled surgical cut, not a traumatic break.
When Do You Still Need a Full Sternotomy?
Despite advances in technology, the median sternotomy remains necessary for many procedures. If your heart problem involves multiple areas, the "open door" approach is safer and more efficient.
You will likely need a full sternotomy if you are having:
- Cabg (Coronary Artery Bypass Grafting): Especially if you need bypasses on three or four vessels. Surgeons need to see the entire surface of the heart to attach grafts properly.
- Complex Valve Replacements: If you need both an aortic and mitral valve replaced simultaneously.
- Aortic Aneurysm Repair: Fixing a bulge in the main artery coming out of the heart often requires direct access to the aorta.
- Heart Transplant: Removing the old heart and implanting a new one requires maximum visibility.
In these cases, trying to squeeze through a small hole between the ribs would be risky. It could prolong the surgery, increase bleeding, or limit the surgeon’s ability to handle complications if they arise. Safety comes first.
The Rise of Minimally Invasive Heart Surgery
This is where things get exciting for patients who want to avoid the sternotomy. Over the last 20 years, minimally invasive cardiac surgery, which is heart surgery performed through small incisions without splitting the sternum, has become mainstream. These techniques allow surgeons to work through gaps between the ribs or through tiny holes drilled in the chest wall.
If you qualify for one of these approaches, you keep your sternum intact. Here are the most common minimally invasive options available in 2026:
Right Anterior Mini-Thoracotomy
For certain valve repairs, especially the mitral valve, surgeons make a small incision (about 4-6 inches) on the right side of the chest, between the ribs. They spread the ribs slightly apart-not breaking them-to insert instruments. Because the sternum is untouched, recovery is faster, and the risk of deep chest infection is lower.
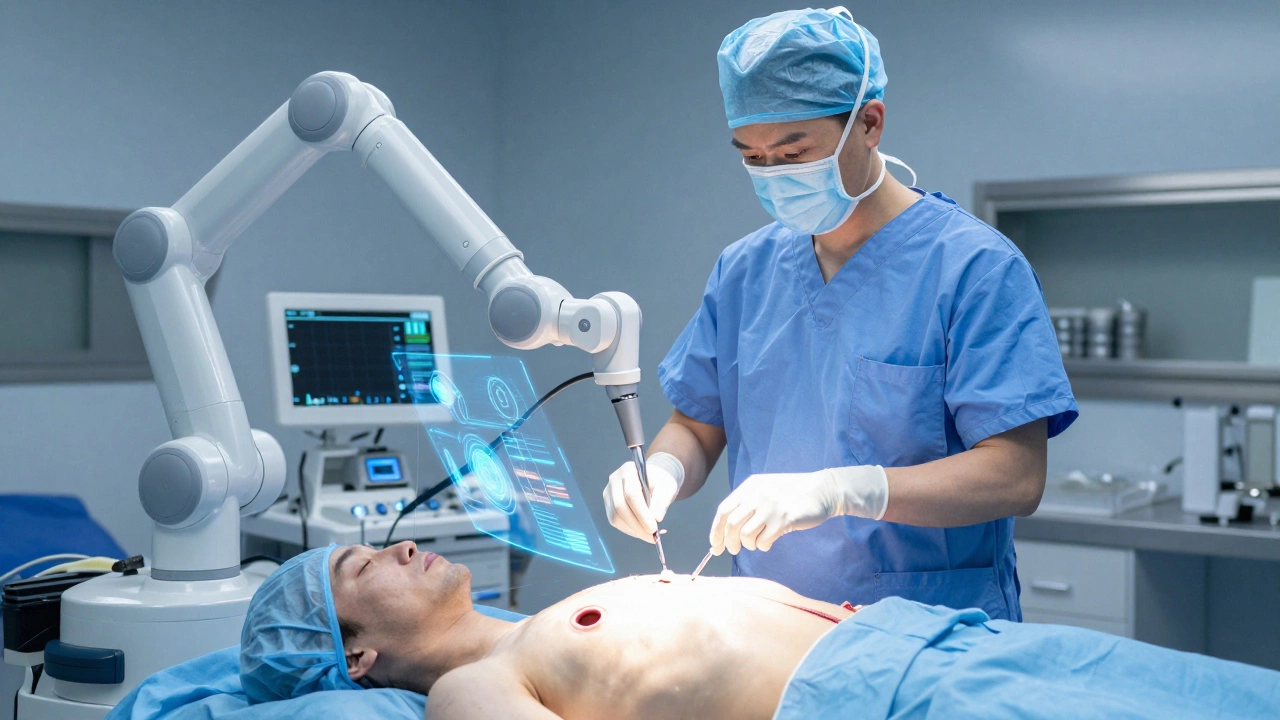
Robotic-Assisted Heart Surgery
Using systems like the da Vinci Surgical System, surgeons control robotic arms through keyhole-sized incisions (about half an inch each). The camera provides a 3D, magnified view of the heart. This is commonly used for mitral valve repair, atrial septal defect closure, and some coronary bypasses. Since there is no large incision, scarring is minimal, and pain is significantly reduced.
Transcatheter Procedures
This is the biggest game-changer. For some conditions, you don’t need open surgery at all. Instead, doctors thread catheters through blood vessels in your groin or wrist and guide them up to the heart.
TAVR (Transcatheter Aortic Valve Replacement), which is a procedure to replace the aortic valve via catheter without open-heart surgery, is now the standard of care for many older adults with severe aortic stenosis. Similarly, MitraClip can repair leaky mitral valves without opening the chest. These procedures often allow patients to go home within 24 to 48 hours.
Comparison: Sternotomy vs. Minimally Invasive Approaches
| Feature | Median Sternotomy | Minimally Invasive / Robotic | Transcatheter (TAVR/MitraClip) |
|---|---|---|---|
| Incision Size | 6-8 inches (vertical) | 2-4 inches or several tiny holes | Small puncture in groin/wrist |
| Bone Impact | Sternum split and wired | Ribs spread slightly; sternum intact | No bone contact |
| Hospital Stay | 5-7 days | 3-5 days | 1-2 days |
| Recovery Time | 6-8 weeks for bone healing | 3-4 weeks | 1-2 weeks |
| Pain Level | Moderate to High | Mild to Moderate | Mild |
| Best For | Multi-vessel CABG, complex multi-valve disease | Single valve repair, ASD closure | High-risk patients, aortic stenosis |
Who Qualifies for Minimally Invasive Surgery?
You might be hoping for the less invasive option, but not everyone is eligible. Your cardiologist and cardiac surgeon will evaluate several factors before deciding on the approach.
Anatomy matters. If your heart is enlarged or your blood vessels are tortuous (twisted), it might be too difficult to navigate tools through small openings. Prior surgeries can also complicate things. If you’ve had open-heart surgery before, scar tissue may make minimally invasive approaches risky.
Surgeon expertise is crucial. Robotic and minimally invasive techniques require highly specialized training. Not every hospital offers these options. You may need to travel to a high-volume center to access them. Cost and insurance can also play a role. While minimally invasive surgery often leads to shorter hospital stays, the equipment costs are higher. Check with your provider to ensure coverage.

Recovery: What to Expect Regardless of Approach
Even if you avoid the sternotomy, heart surgery is still major surgery. Your body has undergone stress, anesthesia, and manipulation of vital organs.
If you had a sternotomy, your biggest concern is sternal stability. You must follow the "no-lifting" rule strictly. Using a pillow to splint your chest when coughing helps reduce pain. Walking is encouraged immediately after surgery to prevent blood clots and pneumonia.
If you had minimally invasive surgery, you’ll still have soreness in the chest muscles where the incisions were made. You won’t have the same restrictions on movement, but you should still take it easy for the first few weeks. Cardiac rehabilitation-a supervised program of exercise and education-is recommended for all patients to improve long-term outcomes.
Pain management has improved dramatically. Multimodal analgesia (using a combination of non-opioid medications, nerve blocks, and low-dose opioids) helps control pain without excessive sedation. This allows you to breathe deeply and move sooner, speeding up recovery.
Questions to Ask Your Surgeon
Don’t assume you’ll get the least invasive option automatically. Have a detailed conversation with your medical team. Here are specific questions to ask:
- "Is my anatomy suitable for a minimally invasive approach?"
- "What are the risks of doing this procedure through a small incision versus a full sternotomy?"
- "How many of these specific minimally invasive procedures have you performed?"
- "Will I need a pacemaker or other devices post-surgery?"
- "What is the expected timeline for returning to normal activities?"
Your surgeon’s experience with a particular technique is just as important as the technique itself. A skilled surgeon performing a sternotomy may offer better outcomes than an inexperienced surgeon attempting a complex robotic procedure.
Final Thoughts on Chest Surgery
The idea that surgeons "break your ribs" is a persistent myth rooted in fear and misunderstanding. In reality, modern cardiac surgery is precise, planned, and tailored to your specific condition. While the sternum is still split for many complex procedures, it is done with precision tools and secured firmly to heal properly.
More importantly, you have options. If your condition allows, minimally invasive or transcatheter techniques can spare you the sternotomy entirely. These advancements mean less pain, shorter hospital stays, and a quicker return to life. Talk to your cardiologist about whether you qualify for these newer approaches. Knowledge is power, and understanding your options reduces anxiety and empowers you to participate in your own care.
Do surgeons break ribs during open-heart surgery?
No, surgeons do not break ribs. In traditional open-heart surgery, they split the sternum (breastbone) using a specialized saw. The ribs themselves remain intact. The sternum is then wired back together to heal.
Can I have heart surgery without splitting my breastbone?
Yes, depending on the procedure. Minimally invasive techniques like mini-thoracotomy or robotic-assisted surgery allow surgeons to work through small incisions between the ribs. Transcatheter procedures like TAVR require no chest incisions at all.
How long does it take for the sternum to heal after surgery?
Sternal healing typically takes 6 to 8 weeks. During this time, you must avoid lifting heavy objects, pushing, or pulling to prevent the wires from breaking or the bone from shifting.
Is minimally invasive heart surgery safer than open-heart surgery?
For selected patients, yes. It offers less blood loss, lower infection risk, and faster recovery. However, it is not suitable for everyone. Complex cases or anatomical limitations may make traditional sternotomy safer and more effective.
What is TAVR and who is it for?
TAVR (Transcatheter Aortic Valve Replacement) is a procedure to replace a narrowed aortic valve using a catheter inserted through the groin. It is primarily for patients with severe aortic stenosis who are at high risk for traditional open-heart surgery, though it is increasingly used in lower-risk patients too.
Will I feel pain after minimally invasive heart surgery?
You will experience some pain and soreness, but it is generally much less than with a sternotomy. Pain is managed with medication, and most patients report being able to manage discomfort well enough to walk and perform light activities soon after discharge.